07 February 2023
An international research team comprised of members from the School of Public Health, LKS Faculty of Medicine of the University of Hong Kong (HKUMed), the Laboratory of Data Discovery for Health (D24H) and the Centre for Immunology & Infection (C2i), in collaboration with the Hong Kong Red Cross Blood Transfusion Service, provided one of the first real-world estimates of vaccine effectiveness against Omicron infections, irrespective of symptoms or severity. Via a serological survey of 5,310 blood donors and other volunteers, the researchers estimated that three doses of the Comirnaty or CoronaVac vaccines were, respectively, 48% or 30% effective in preventing Omicron infection shortly after vaccination, further improving shortly after a fourth dose. The researchers expected protection from infection also relates to protection from transmission, and this is one of the first reports suggesting vaccine-induced protection from Omicron virus transmission. However, vaccine effectiveness waned rapidly thereafter over 100 days. Moreover, the researchers estimated that more than 45% of the Hong Kong population was infected between 1 January and 31 July 2022. The findings are now available on Nature Medicine [link to the publication].
Background
The SARS-CoV-2 Omicron variant has demonstrated enhanced transmissibility and escape of vaccine-derived immunity. Between 1 January to 31 July 2022, Hong Kong experienced an unprecedented fifth wave of COVID-19 infections driven predominantly by the Omicron BA.2 subvariant. As local COVID transmission before 2022 was minimal, population immunity to SARS-CoV-2 in Hong Kong was almost entirely vaccine-derived at the start of the wave.
There is extensive data on how COVID-19 vaccines robustly prevent severe disease, hospitalisation and death. However, few studies have investigated their effectiveness in preventing Omicron infections, irrespective of symptoms or severity. Prevention of infection itself indicates prevention of both asymptomatic and symptomatic disease transmission.
Research methods and findings
Combining results from a community-wide serological survey of 5,310 blood donors and volunteers with SARS-CoV-2 viral load data from city-wide wastewater surveillance, the researchers estimated, (i) vaccine effectiveness against all Omicron BA.2 infections conferred by two, three and four homologous doses of the Comirnaty or CoronaVac vaccines for 100 days after each dose and (ii) COVID-19 infection attack rate in Hong Kong from 1 January to 31 July 2022. The researchers developed two in-house ELISA assays detecting IgG antibodies to the nucleocapsid (N) or Open Reading Frame 8 (ORF8) protein of SARS-CoV-2, with the latter assay developed specifically to detect past infection in CoronaVac vaccines.
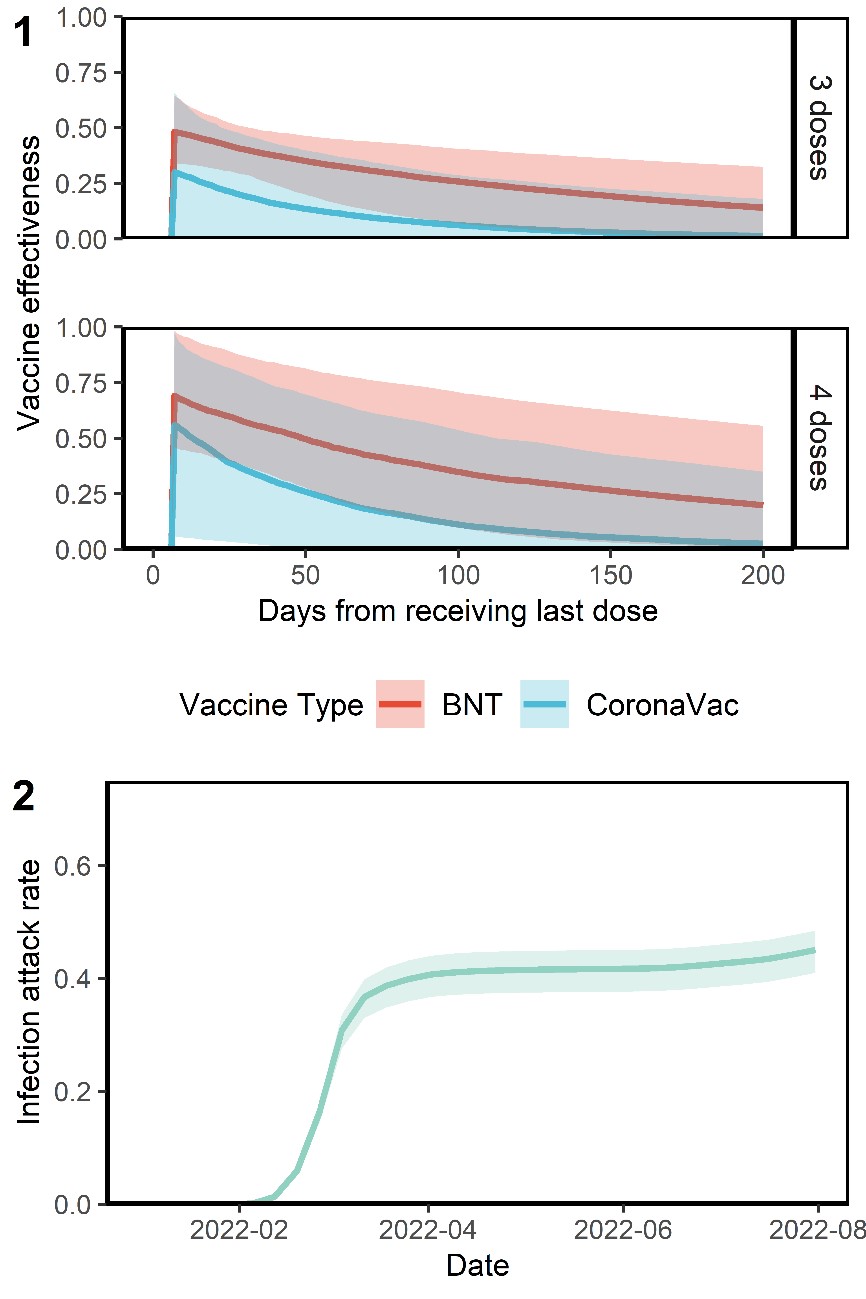
The researchers estimated three and four doses of Comirnaty were 48% and 69% effective in preventing Omicron infection, respectively, 7 days after vaccination, waning to 26% and 35% by 100 days after vaccination. Three and four doses of CoronaVac were 30% and 56% effective after 7 days respectively, declining to 6% and 11% by 100 days.
Meanwhile, the researchers identified that more than 45% of the local population in Hong Kong was infected by SARS-CoV-2 between 1 January and 31 July 2022 (i.e. an infection attack rate of 45%). Accordingly, official case counts, incorporating both Reverse Transcriptase-PCR (RT-PCR) testing and Rapid Antigen Testing (RAT) results, identified less than 41% of all infections.
Significance of the study
The results indicate that booster vaccination using either the mRNA or inactivated vaccine platforms is effective in preventing SARS-CoV-2 Omicron BA.2 infection in the short-term. This adds to previous studies demonstrating robust vaccine effectiveness in preventing severe disease and death.
Thus, surge booster campaigns, particularly with updated bivalent mRNA vaccines, could be strategically used to rapidly boost population immunity when there is risk of future waves of infections arising from a concerning novel virus variant. The comparatively lower infection attack rate in Hong Kong by July 2022, versus various overseas jurisdictions, highlights the effect of supplementing vaccination campaigns with continued public health and social measures (e.g. masking) on reducing disease transmission.
About the research team
This study was co-led by Professor Joseph Wu Tsz-kei, School of Public Health, HKUMed and Managing Director and Lead Scientist, the Laboratory of Data Discovery for Health (D24H) and Professor Malik Peiris, School of Public Health, HKUMed and Co-Director, the Centre for Immunology & Infection (C2i). The research team also included Professor Gabriel Leung, Honorary Clinical Professor, School of Public Health, HKUMed and Chief Scientific Officer Emeritus, D24H; Dr Cheuk-Kwong Lee, Hong Kong Red Cross Blood Transfusion Service, Hospital Authority; Professor David Hui Shu-cheong, The Jockey Club School of Public Health and Primary Care, CU Medicine, the Chinese University of Hong Kong; Professor Gaya Amarasinghe, Department of Pathology & Immunology, Washington University in St. Louis, USA; Dr Eric Lau Ho-yin, School of Public Health, HKUMed; Dr Kathy Leung Sze-man, School of Public Health, HKUMed; Dr Sophie Valkenburg, Peter Doherty Institute for Infection and Immunity, University of Melbourne and HKU-Pasteur Research Pole, HKUMed; Dr Masashi Mori, Ishikawa Prefectural University, Japan; Dr Chao Wu, Department of Pathology & Immunology, Washington University in St. Louis, USA; Jonathan Lau, Samuel Cheng, Leo Tsang, Kenny Yam, Sara Chaothai, Kelvin Kwan, Zacary Chai and Tiffany Lo, all of the School of Public Health, HKUMed and Asmaa Hachim, HKU-Pasteur Research Pole, HKUMed.
Acknowledgements
The researchers thank the Hong Kong Red Cross Blood Transfusion Service and the 5,310 blood donors and community volunteers for their support and participation. The researchers also thank the following agencies of The Government of the Hong Kong Special Administrative Region (HKSAR) for research support: Office of the Government Chief Information Officer, Department of Health, Centre for Health Protection and Environmental Protection Department. This study was supported by the Health and Medical Research Fund, Health Bureau (COVID190126), AIR@InnoHK and C2i, administered by the Innovation and Technology Commission of the Government of the HKSAR, and the Theme-based Research Grants Scheme of the HKSAR.
Media enquiries
Please contact LKS Faculty of Medicine of The University of Hong Kong by email (medmedia@hku.hk).

Follow HKUMed